Patient Education
Heart Health Library
Our Health Library does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their heart health. Our providers may not see and/or treat all topics found herein.
Our Health Library information does not replace the advice of a doctor. Please be advised that this information is made available to assist our patients to learn more about their health. Our providers may not see and/or treat all topics found herein.
Mastitis While Breastfeeding
Condition Basics
What is mastitis?
Mastitis is a breast inflammation sometimes caused by infection. It can happen at any time. But it's most common during the first 6 months of breastfeeding (sometimes called chestfeeding). It is especially common during the baby's first 2 months. After 2 months, the baby's feeding patterns become more regular, which helps prevent mastitis.
Mastitis can be painful and make you very tired. But it is usually easily cleared up with self-care and sometimes antibiotics. You can continue to safely breastfeed your baby while you have mastitis. In fact, breastfeeding usually helps to clear up mastitis.
What causes it?
Mastitis can happen when the milk ducts narrow and do not drain properly. This can cause swelling and inflammation in the breast. And sometimes the tissue can become infected with bacteria. Infection is more likely to occur if you have cracked or sore nipples.
What are the symptoms?
If you have mastitis, you may first notice:
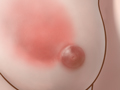
- Pain, swelling, or warmth on an area of your breast. And the skin may be reddish, purplish, or brownish, depending on your usual skin color.
- Chills, aches, and flu-like symptoms.
- A fever.
Signs that mastitis is getting worse include swollen and painful lymph nodes in the armpit next to the infected breast, a fast heart rate, and flu-like symptoms that get worse. Mastitis can lead to a breast abscess, which feels like a hard, painful lump.
The symptoms of mastitis most often appear within 4 to 6 weeks after childbirth.
How is it diagnosed?
Your doctor or midwife can usually diagnose mastitis based on your symptoms and by checking your affected breast. Tests usually aren't needed.
How is mastitis treated?
Treatment for mastitis includes regular breastfeeding and self-care. If you have an infection, you will likely need antibiotics. Self-care includes taking ibuprofen (Advil, Motrin) and using cold compresses for discomfort and swelling. Treating mastitis right away with self-care can help keep it from getting worse and usually eases symptoms.
Prevention
Taking these steps can help prevent mastitis.
- Breastfeed regularly. This helps keep milk moving. If you know you'll go more than 4 hours without feeding your baby, arrange to pump. But limit pumping if you can. Try to only pump when you need to. Pumping more than your baby needs may make mastitis worse.
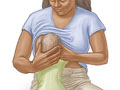
- Position yourself well. When you and your baby are aligned, the baby can latch on to the areola, not just the nipple.
- Use different positions. This can help drain all areas of your breast. Try breastfeeding positions such as the Australian hold, the cradle hold, the cross-cradle hold, the football hold, and the side-lying position.
- Alternate which breast you offer first.
- Wear a supportive bra that fits.
- Take care of your nipples.
- Air-dry your nipples after you breastfeed. This can prevent irritation and cracking.
- Try letting some breast milk dry on your nipples if they are sore.
- Get help from your doctor or midwife or a lactation consultant for sore or cracked nipples.
- Avoid massaging your breasts. This can cause tissue injury and increase inflammation.
- When you are ready to wean your baby, do it gradually. Gradual weaning helps prevent your breasts from getting too full.
Learn more
Symptoms
If you have mastitis, you may first notice:
- Pain, swelling, or warmth on an area of your breast. And the skin may be reddish, purplish, or brownish, depending on your usual skin color.
- Chills, aches, and flu-like symptoms.
- A fever.
These first symptoms may start after you have reopened a blocked milk duct.
Signs that mastitis is getting worse include swollen and painful lymph nodes in the armpit next to the infected breast, a fast heart rate, and flu-like symptoms that get worse.
The symptoms of mastitis most often appear within 4 to 6 weeks after childbirth.
In some cases, symptoms of mastitis get worse and the breast forms a pocket of pus (abscess) in the infected area.
Symptoms of a breast abscess
Symptoms of a breast abscess include a breast lump that is hard and painful. The area may be reddish, purplish, or brownish, depending on your usual skin color. You may also have flu-like symptoms that are getting worse.
Exams and Tests
Your doctor or midwife can usually diagnose mastitis based on your symptoms and by checking your affected breast. Tests usually aren't needed. But tests may be done to confirm a diagnosis. They may also be done to help guide treatment for other problems that can develop.
If you have an infection that isn't improving with treatment, your doctor or midwife may do a breast milk culture. To provide a sample for a culture, you will squeeze a small sample of milk from the affected breast onto a sterile swab. The culture results help your doctor or midwife confirm a diagnosis and find out the specific bacteria causing the infection.
Culture results may also be used to find out which antibiotic will work best for you.
Diagnosing a breast abscess
Your doctor or midwife can diagnose a breast abscess by checking your breast. If an abscess is deep, your doctor or midwife may use a breast ultrasound to check it. Ultrasound can also guide a needle to drain the abscess. A culture can then be done to identify the bacteria causing the abscess.
Learn more
Treatment Overview
Mastitis may go away with early self-care and management of symptoms. Sometimes you will need antibiotics. Treating it right away helps keep it from quickly getting worse and usually eases symptoms after about 2 days. Delaying treatment can lead to an abscess, which can be harder to treat.
Treatment may include:
- Regular breastfeeding. This helps keep milk moving. Be sure to breastfeed from both breasts.
- Self-care. This can include taking ibuprofen (Advil, Motrin) or using a cold compress to reduce pain and swelling, changing your breastfeeding positions, and resting as needed.
- Taking antibiotics. They can treat infection if you have one.
You can safely keep breastfeeding your baby during illness and treatment. Your breast milk is safe for your baby to drink. Any bacteria in your milk will be destroyed by the baby's digestive juices.
Treating a breast abscess
Treatment for a breast abscess includes:
- Draining the abscess. Healing can take 5 to 7 days.
- Antibiotics that you take by mouth. They destroy the bacteria that are causing the infection. Antibiotics are given through a vein (intravenously) only in rare cases of severe infection.
- Breastfeeding regularly. This is also very important for keeping a good milk supply.
Most people can keep breastfeeding with the affected breast while an abscess heals. With your doctor's or midwife's approval, you can cover the abscess area with a light gauze dressing while you breastfeed.
If you are told to stop breastfeeding from the affected breast while an abscess heals, you can keep breastfeeding from the healthy breast. Be sure to pump or express milk from the infected breast regularly.
Learn more
Self-Care
- Continue to regularly breastfeed when your baby is hungry.
- Limit pumping if you can. Try to only pump when you need to. Frequent pumping may make mastitis worse.
- Hand express a little before breastfeeding if your breasts are very full (engorged). This may make it easier for your baby to latch.
- Try taking ibuprofen (Advil, Motrin) for pain and swelling.
- Rest as much as you can.
- Use a cold compress for pain and swelling.
- Put ice or a cold pack on the area for 10 to 20 minutes at a time. Put a thin cloth between the ice and your skin.
- Take care of your nipples.
- Let your nipples air dry after feeding. Try letting some breast milk dry on your nipples if they are sore.
- Avoid using saline soaks or castor oil on your affected breast or on sore nipples. Ask your doctor before you use any other products on your breast.
- Try applying a nonstick first-aid pad to your breasts after each feeding.
- Avoid massaging the breast. This can cause tissue injury and worsen swelling.
- Wear a supportive bra that fits.
If you have trouble breastfeeding, talk to your doctor or midwife or a lactation consultant.
Breastfeeding when you have mastitis
Regular breastfeeding is an important part of caring for yourself when you have mastitis. If you have any problems with breastfeeding, talk to your doctor or midwife or a lactation consultant.
- Regularly breastfeed when your baby is hungry. Your milk is safe for your baby to drink. Your baby's digestive juices will destroy any bacteria in your milk.
- Try to start on the sore side.
- If you need to start on the other side, be sure to switch and breastfeed from the affected side as well.
- Vary your breastfeeding positions to help drain different areas of your breasts.
- If it's too painful to breastfeed at all, you can pump or express your milk.
- Take care of your nipples.
- Let your nipples air dry after feeding.
- Try letting some breast milk dry on your nipples if they are sore. Some people try an over-the-counter lanolin-based cream, such as Lansinoh.
- If your nipples are cracked and bleeding, try applying a nonstick first-aid pad to your breast after each feeding.
- Replace nursing pads often. Dry and clean pads are best.
Learn more
Related Information
Credits
Current as of: April 30, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: April 30, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
This information does not replace the advice of a doctor. Ignite Healthwise, LLC disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use and Privacy Policy. Learn how we develop our content.
To learn more about Ignite Healthwise, LLC, visit webmdignite.com.
© 2024 Ignite Healthwise, LLC. Healthwise, Healthwise for every health decision, and the Healthwise logo are trademarks of Ignite Healthwise, LLC.
Heart Topics
Browse our library of medical conditions and treatments
Interactive Tools
Tips on how to stay healthy